What is the risk of stroke from chiropractic neck adjustments?
Understanding the Chiropractic Stroke Risk Debate
Few topics in healthcare generate as much discussion — and concern — as the potential link between chiropractic neck adjustments and stroke. For decades, patients, physicians, and chiropractors have debated whether cervical spine manipulation carries a meaningful risk of triggering a serious neurological event. If you have ever wondered whether that satisfying “crack” during a neck adjustment could have dangerous consequences, you are not alone.
This article takes a careful, evidence-based look at what the research actually says about the chiropractic stroke risk, who may be most vulnerable, and how to make an informed decision about your care.
How Could a Neck Adjustment Cause a Stroke?
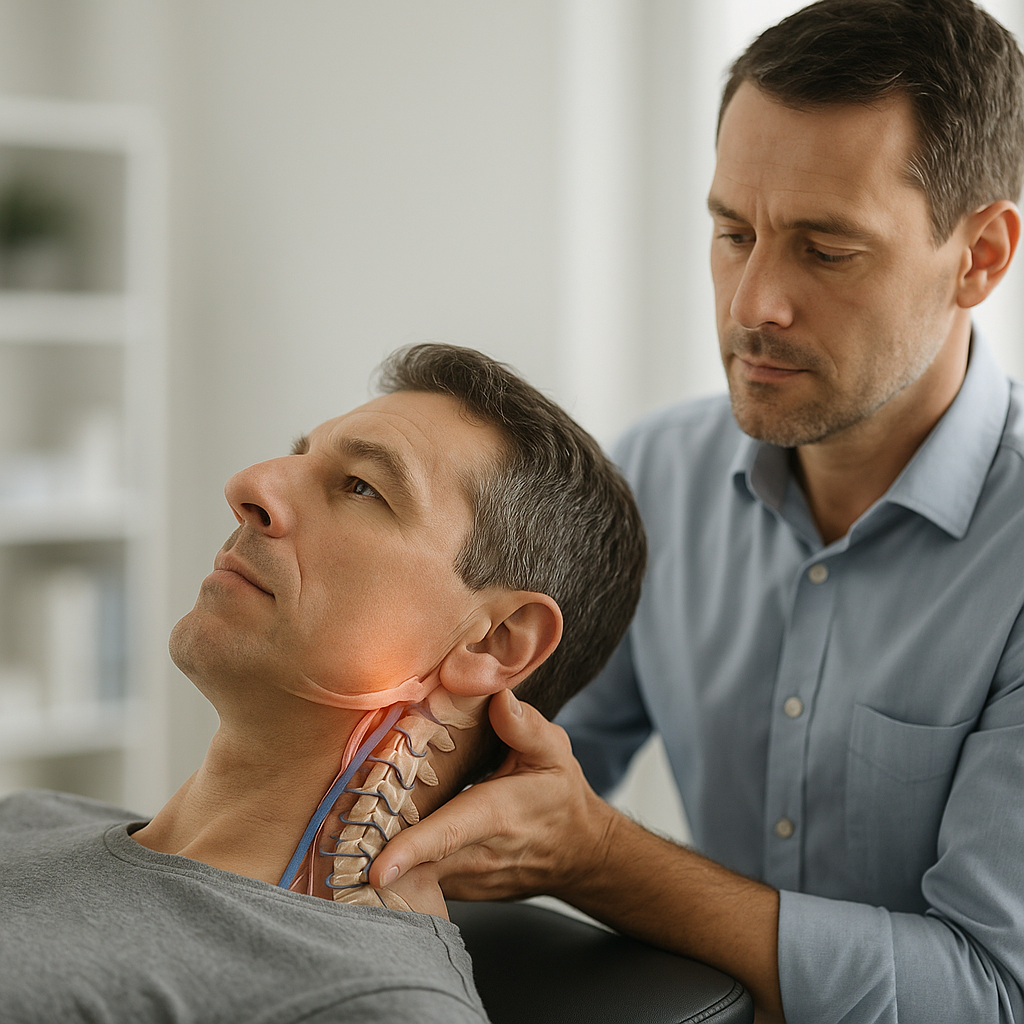
To understand the concern, it helps to understand the anatomy involved. Running along either side of the cervical spine (the neck vertebrae) are two blood vessels called the vertebral arteries. These arteries travel through small openings in the vertebrae before entering the skull, where they merge and supply blood to the brainstem and cerebellum — areas responsible for coordination, balance, breathing, and other vital functions.
The proposed mechanism of harm is known as vertebral artery dissection. During a chiropractic neck adjustment — particularly high-velocity, low-amplitude (HVLA) thrust techniques — the rapid rotational movement of the cervical spine could theoretically stretch or tear the inner lining (intima) of the vertebral artery. This tear can lead to:
- The formation of a blood clot at the site of the injury
- Pieces of that clot breaking off and traveling to the brain
- Blockage of blood flow to critical brain structures
- A posterior circulation stroke, sometimes called a vertebrobasilar stroke
This sequence of events — cervical manipulation stroke — though theoretically plausible, is at the heart of an ongoing scientific controversy about how frequently it actually occurs and whether chiropractic care is truly the cause.
What Does the Research Say About the Risk?
Quantifying the actual chiropractic stroke risk has proven surprisingly difficult. Studies have produced a wide range of estimates, and methodological limitations make definitive conclusions elusive. Here is a summary of what the current body of evidence suggests:
Early Estimates Were Alarming — But May Have Been Misleading
Early case reports and observational studies from the 1990s and early 2000s suggested that vertebral artery dissection following chiropractic manipulation occurred somewhere between 1 in 20,000 and 1 in 1,000,000 cervical manipulations. These wide ranges reflected the inherent difficulty in tracking adverse events across a large and decentralized healthcare profession.
The Confounding Factor: Were Patients Already Having Strokes?
A critical insight emerged from a landmark 2008 study published in Spine and subsequent research: people in the early stages of a vertebral artery dissection often experience neck pain and headache as their first symptoms. This means that a patient with a stroke already in progress might seek chiropractic care for neck pain — and then suffer a stroke shortly afterward — creating the appearance of a causal link when the relationship may simply be coincidental.
In other words, the chiropractor’s office may be the last stop before a stroke that was going to happen regardless. This phenomenon, known as presenting bias or confounding by indication, has significantly complicated the interpretation of observational data linking neck adjustment to stroke.
Population-Level Studies Offer Reassurance — With Caveats
Several large-scale population studies have attempted to control for this confounding factor. A widely cited study using Ontario health insurance data found that the association between chiropractic visits and vertebrobasilar stroke was no greater than the association between visits to a primary care physician and the same type of stroke — suggesting that the apparent risk may be an artifact of patients seeking care for early stroke symptoms rather than evidence of causation.
However, critics of these studies point out that they rely on administrative data, which may not capture the nuances of specific manipulation techniques, patient risk factors, or the clinical details that would help disentangle cause and effect.
Who Is at Greatest Risk?
While the absolute risk remains debated, researchers and clinicians have identified certain characteristics that may make some individuals more vulnerable to vertebral artery dissection — whether from chiropractic manipulation or other activities. Risk factors for vertebral artery dissection chiropractic-related or otherwise include:
- Pre-existing arterial abnormalities: Conditions such as fibromuscular dysplasia, connective tissue disorders (like Marfan syndrome or Ehlers-Danlos syndrome), or atherosclerosis may weaken arterial walls.
- Recent trauma: A prior injury to the neck — even a minor one — may have already compromised arterial integrity.
- Hypertension: Chronically elevated blood pressure can weaken blood vessel walls over time.
- Migraine with aura: Some research suggests an association between migraines and arterial vulnerability.
- Young age: Counterintuitively, vertebral artery dissection strokes most commonly affect adults between the ages of 35 and 50, rather than older individuals.
- Blood clotting disorders: Conditions that affect how blood clots form or dissolve may increase risk.
It is worth noting that vertebral artery dissection can also be triggered by far more mundane activities, including turning the head sharply, coughing, sneezing, painting a ceiling, or even certain yoga poses. This puts the chiropractic-specific risk in a broader perspective.