What is a range of motion test in chiropractic?
Understanding Range of Motion Testing in Chiropractic Care
When you visit a chiropractor for the first time, or even as part of an ongoing treatment plan, one of the most fundamental assessments you are likely to encounter is a range of motion test. This evaluation serves as a cornerstone of chiropractic diagnosis and helps practitioners develop targeted, effective treatment strategies. Understanding what a ROM test chiropractic evaluation involves — and why it matters — can help you feel more confident and informed during your care journey.
What Is a Range of Motion Test?
A range of motion (ROM) test is a clinical assessment used to measure how far a joint or group of joints can move through their natural arc of movement. In the context of chiropractic care, this typically involves evaluating the spine, hips, shoulders, neck, and other key joints throughout the body. The test determines whether a patient’s joint mobility falls within a normal, healthy range or whether restrictions, stiffness, or abnormal movement patterns are present.
The results of a range of motion evaluation provide chiropractors with objective, measurable data that forms the foundation of an accurate diagnosis. Rather than relying solely on a patient’s subjective description of pain or discomfort, ROM testing gives practitioners a quantifiable picture of how the body is actually functioning.
Why Is Range of Motion Important in Chiropractic?
Joint flexibility and mobility are essential to overall musculoskeletal health. When a joint’s range of motion is restricted, it can lead to compensatory movement patterns, muscle imbalances, chronic pain, and reduced quality of life. A thorough joint flexibility test allows chiropractors to:
- Identify specific areas of restriction or dysfunction within the musculoskeletal system
- Detect asymmetries between the left and right sides of the body
- Establish a baseline for tracking progress over time
- Differentiate between various conditions that may present with similar symptoms
- Formulate a personalized, evidence-based treatment plan
- Evaluate the effectiveness of ongoing chiropractic interventions
Without this information, treatment would be far less precise. ROM testing ensures that chiropractic care is not only appropriate for the patient’s condition but also that it is being applied with the right level of intensity and focus.
How Is a ROM Test Performed in a Chiropractic Setting?
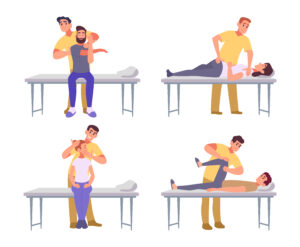
A spinal mobility assessment and broader range of motion evaluation are typically performed in a systematic, structured manner. Depending on the area being assessed, the chiropractor may use one or more of the following approaches:
Active Range of Motion (AROM)
In this component of the test, the patient is asked to move the joint independently, without any assistance from the practitioner. For example, the patient may be instructed to tilt their head forward and backward, rotate their trunk from side to side, or raise their arms overhead. Active range of motion testing reveals how much movement the patient can perform under their own muscular control and highlights areas where pain or weakness may be limiting function.
Passive Range of Motion (PROM)
During passive testing, the chiropractor gently moves the patient’s joint through its range of motion without the patient exerting any effort. This approach helps isolate the structural capacity of the joint itself, independent of muscular strength or neurological control. It is particularly useful for identifying joint capsule restrictions, ligamentous tightness, or bony limitations.
Resisted Range of Motion (RROM)
In this variation, the patient attempts to move the joint while the chiropractor applies a controlled opposing force. This method is valuable for assessing muscular strength and detecting conditions such as tendon injuries or nerve compression that may be affecting a patient’s ability to generate movement.
Measuring and Documenting Range of Motion
Precise measurement is critical to a meaningful range of motion evaluation. Chiropractors typically use a device called a goniometer — a protractor-like instrument designed to measure joint angles accurately. In more advanced clinical settings, inclinometers and digital measurement tools may also be used to ensure consistency and accuracy.
The measurements obtained are compared against established norms for each joint and movement plane. For instance, normal cervical flexion (bending the neck forward) is generally considered to be approximately 45 to 50 degrees, while lumbar flexion (bending the lower back forward) is typically around 60 degrees. Any significant deviation from these benchmarks is noted and factored into the diagnostic picture.
Documentation of ROM findings is equally important. Chiropractors record these measurements carefully so that future assessments can be compared, allowing both the practitioner and patient to see tangible evidence of improvement or to identify areas requiring additional attention.
Which Areas Are Commonly Assessed in a Chiropractic ROM Test?
A comprehensive ROM test chiropractic evaluation may focus on multiple regions depending on the patient’s complaint and presentation. The most commonly assessed areas include:
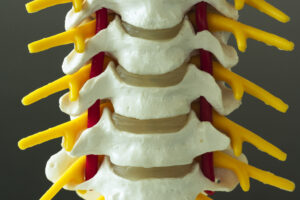
- Cervical Spine (Neck): Flexion, extension, lateral flexion, and rotation are all evaluated to identify neck stiffness or injury-related restrictions.
- Thoracic Spine (Mid-Back): Rotation and lateral flexion are the primary movements assessed in this region, often in relation to posture or rib-related complaints.
- Lumbar Spine (Lower Back): Flexion, extension, and lateral bending are carefully measured, particularly in patients presenting with lower back pain or sciatica.
- Shoulder Joint: A full shoulder assessment includes elevation, abduction, internal and external rotation, and horizontal adduction.
- Hip Joint: Hip flexion, extension, abduction, adduction, and rotational movements are all part of a thorough evaluation, especially in patients with lower limb or pelvic complaints.